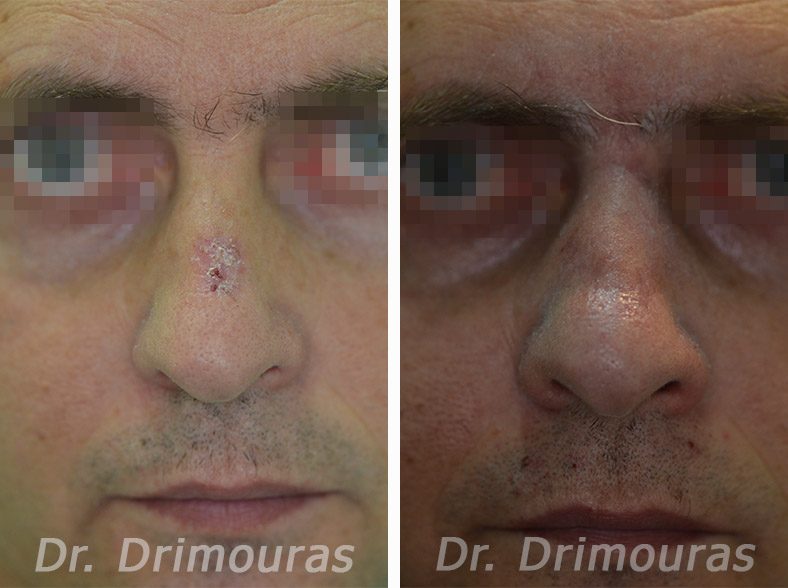
Precancerous Lesions
The term “precancerous lesions” refers to diseases that appear with an elevated risk of developing cancer. With an early and appropriate treatment, we succeed in having high percentages of cure.
Actinic Keratosis & Actinic Cheilitis
The term refers to conditions which are a result of long-term accumulating harmful effect of sunlight. They are usually observed at ages over 40 and are slightly more frequent to men. People who have fair skin, that do not react with “normal” tanning when exposed to solar radiation develop those lesions more often. On the contrary, dark-skinned individuals scarcely develop actinic keratosis. This fact is related to the protection that melanin provides to the skin.

The lesions are usually detected on the face, scalp, neck, dorsal surface of the hand, arms and rarely on the back, shoulders and shins. A body part where the lesions are often diagnosed is the lower lip, where deteriorations caused from chronic exposure to the sun are called actinic cheilitis.
Deteriorations increase in size as time passes. It is estimated that one out of five patients (20%) with actinic lesions develops a squamous cell carcinoma These carcinomae become metastatic in 0,5-3 out of 100 cases. The possibility of metastasis increases to a percentage of 11% when it comes to squamous cell carcinomae detected on the lower lip or on auricle of the ear.
Actinic lesions, when superficial, may be treated with cryotherapy, electrocauteration or CO2 laser. In deep, thick lesions, that do not respond to the aforementioned treatments, and in those detected on the lower lip and ear auricle, it is safer to treat with surgical removal and biopsy.
Early diagnosis and treatment of those precancerous lesions protect patients from the development of an infiltrative carcinoma. Prevention remains an essential parameter and sunscreen protection should begin from a human’s birth.
Keratoacanthoma
The keratoacanthoma is a relatively ordinary tumor, which causes worry to the patient due to its speedy growth. It often poses a problem of differential diagnosis with its highly malignant squamous cell carcinoma. It appears on the face at a percentage of 70%, on the palmar surface of the hands at a percentage of 15-20% and more seldom on the chest, thigh, shoulder and perigenital area.

Causative factors involved in the pathogenity of the keratoacanthoma are solar radiation, X and PUVA rays, chemical carcinogens, trauma, smoking, genetic factors, infectious and immunological (immunosuppression) factors.
The typical course of a keratoacanthoma is characterized by the rapid growth phase (1-2 months), the stage of tranquility where the development of the severe damage stops (1-2 months) and the stage of spontaneous regression during which the damage gradually reduces in size (2-7 months). One out of five cases does not follow the aforementioned growth pattern. The damage may continue increasing in size; it may also develop an aggressive attitude as an invasive squamous cell carcinoma.
So the reasonable question is: what is the necessity of treatment if there is a spontaneous regression? Therapeutic intervention is necessary for many reasons. Firstly, the aesthetic result after the treatment is more acceptable than the deformed scar of the spontaneous regression. Secondly, the surgical operation of the removal is combined with tissue histological examination for the confirmation of the diagnosis. Thirdly, since the aggressiveness of the lesion cannot be foreseen, treatment speeds up the healing, decreases the time that it remains as an abnormal damage and prevents any destruction of important structures of the face. Fourthly, without treatment, close, long-term observation is required, without being able to rule out the possibility of a malignant change or a metastasis.
Total surgical removal is the usual way of treatment. This method provides suitable material for biopsy and offers a definitive treatment with a good aesthetic result. With the appropriate diagnostic and therapeutic approach an excellent prediction is ensured.
Cutaneous Corn
The cutaneous corn is a hyperkeratotic conical projection on the surface of the skin. It appears mainly on men between the sixth and seventh decade of their lives. The lesion is more often detected on the skin of solar radiated areas of the body, mainly on the face, on the auricle of the ears and on the dorsal surface of the hands. This is connected in most circumstances with the destruction which has been made on the skin with the long term effect of solar radiation. It is less appeared on non-solar exposed areas.

On the base of the skin corn it may be observed, with a histological examination, a range of skin lesions, the most frequent are actinic keratosis (30-40%), warts, (30%), seborrheic keratosis (16%) and the squamous cell carcinomas (20%). The infiltrative carcinomas which are developed on skin corns rarely give metastasis.
Skin corn’s treatment involves surgical removal including the excision of the base on safe surgical margins, followed by histologic examination, combining the diagnosis and treatment.
Chondrodermatitis Nodularis Helicis
Chondrodermatitis nodularis helicis is about exceptional sensitive and persistent lesion, which usually is detected on the horizontal part of the helix of the ear. It appears on people over 40 years old, more often on men. In most cases women are contracted by the lesion on the antihelix of the ear. The pain is acute and during the day it remits slightly. The pressure applied by the pillow exacerbates the pain, forcing the patient to change the side and affecting the quality of sleep.

The etiology for the lesion is not known, however it seems that it is due to long term harmful effects of solar radiation and the pressure applied to this area, in coordination to poor vascularization and slow healing of the ears helix.
During treatment measures must be taken to avoid any pressure on the affected area so as to improve its healing. The local treatment with corticosteroids may help palliative. The only radical therapy is the surgical excision, following by histological examination. After the removal of lesion, the patients must be under observation regularly, because the percentages of relapse remain high.
Bowen’s Disease
The term refers to an intraepidermic (“in situ”) carcinoma of the skin. It affects men slightly more often than women. It appears on exposed or relatively safe from the sum areas of the skin. The lesions may be caused by sunlight, other types of radiation, chemical substances or the viruses of the human papillomas (HPV – Human Papillomavirus).

This disease initially pursues a slow and benign course (horizontal phase of development) for months or years. In the end, the cancer cells infiltrate the dermis as the disease evolves to infiltrative squamous cell carcinoma (vertical phase of development). These carcinomas metastasize to a percent of 5-15%.
The treatment of choice is surgical excision and simultaneously following by histologic examination of surgical margins to confirm whatever malignant tumor has been removed. Other methods like electrocauterization, laser CO2, cryosurgery, 5- fluorouracil and the local use of retinoic acid are not so effective because the cancer cells extend to the adnexal structures of skin with a high rate of recurrence. After the removal of the lesion, the patient must be examined frequently.
Nevus Sebaceous of Jadassohn
Refers to congenital lesion where on all occasions is already visible on the newly born or is developed during early childhood. It is located more often on the scalp, on forehead or postauricular area.


The nevus sebaceous of Jadasshon remains stable during childhood while at the beginning of puberty there appear significant changes. Depending on the area of its detection it may cause aesthetic problems to the patient.
While the possibility of malignant spreading during adulthood of patient is quite large (3-20 %), preventive surgical excision and biopsy of the lesion is recommended.
Leukoplakia
Leukoplakia is a descriptive clinic term and refers to white spots or plague of the oral mucosa, for which biopsies have not been executed yet and for this reason definite diagnosis has not been confirmed. There is an increased danger of malignant transformation of the lesion in the course of time especially when it is detected on the bottom surface of the tongue or on the floor of the oral cavity. The factors that foster the malignant transformation are smoking, chronic trauma, alcohol, ultraviolet radiation and some types of the human papilloma virus (HPV).

Patients should interrupt the use of any smoking products. Clinical follow-up and biopsy of the oral mucosa is recommended on a regular basis. If an epithelial dysplasia is determined, the lesion maybe dealt with cryosurgery, electro-cautery or with topical application of 5- fluorouracil. Intraepidermal (“in situ”) and invasive squamous cell carcinoma must be dealt with excision by surgery and histologic examination. After the surgery close follow up is required, in which an examination of the regional lymph nodes is included.
Erythroplakia of Queyrat
Erythroplakia of Queyrat is about clinical disease of the mucous, which histologically presents the image of intraepidermic (“in situ”) carcinoma. The most frequent detection is under the foreskin of the penis, on people who have not been submitted to circumcision. Least appeared positions of detection of this lesion are the tongue, oral and vaginal mucosa.
The factors that predispose to the penal development of the disease are the sebum, inadequate local sanitation, regression of herpes simplex virus of the genitals, high temperature conditions, mechanical friction and injuries.
It is possible that the disease may persist after many years. Erythroplakia of Queyrat is defined with a greater tense of infiltrative carcinoma development, in comparison to the Bowen’s disease. These squamous cell carcinomas metastasize to a percentage of 10 -30%. Lesions that clinically do not resemble the carcinoma may give metastasis.
Surgical removal is considered the treatment of choice and at the same time a histological examination is always required for clarification of the malignant or non-malignant nature of the lesions.
Chronic Actinic Dermatitis
Chronic actinic dermatitis refers to chronic lesions which appear secondary to radiotherapy or after exposure to ionize radiation for occupational reasons. These chronic deteriorations are a result of harmful effects of ionized radiation on a cellular level. Affected cells lose either partially or totally the ability of division or reproduction.
Degeneration and edema are observed on the skin which appears as a crumbly and atrophic skin surface. On the dermis appears cell dilution, mainly of the fibroblasts, resulting on decreased endurance and elasticity of the skin. On vascular tissue it presents thickening and fibrosis which leads to decreased vascular perfusion with serious healing problems. The subcutaneous fat is also affected and becomes atrophic. The follicles of hair also suffer resulting in thinning of hair line or total losing of hair. Also sebaceous and sweat glands are affected. As a consequence the skin surface becomes dry and rough.
Atrophy of tissue from radiation finally ends up to ulceration. The ulcer appear in the course of 5-20 years from the moment of radiotherapy and it usually begins as a minor injury. The possibility of development of cancer on a skin with radiotherapy after the passing of many years is increased. The most frequent tumors that appear are basal and squamous cell carcinomas. Squamous cell carcinomas which develop on the ground of a radiated area are considered as bad biological behavior and prediction because they often give metastasis. Less frequent appears a sarcoma which also has bad prediction.
The first therapeutical approach must be conservative treatment of ulcers. In the case where these ulcers do not show signs of improvement after a few weeks or when there is a confirmation of malignant transformation, the only effective therapy is the radical surgical removal of involved tissues. The excision includes all the radiated area. The reconstruction of the tissue defect is done with a flap of rich vascular perfusion.
Xeroderma Pigmentosum
Xeroderma pigmentosum is a rare and serious hereditary disease in which cutaneous effects are mainly appeared as multiple skin tumors. These people have an epidermal cell incompetency to repair the damage which is provoked by ultraviolet radiation in their DNA.
Firstly the areas exposed to sunlight react with the appearance of intense erythema. Later small dark spots-freckles appear. Small diameter atrophic skin zones are blended with hypopigmented lesions. These are covered with spider veins and therefore form a diverse image typical of the disease.
The appearance of tumors mostly modifies the course of the disease. 45-62 percent of these people develop basal cell or squamous cell carcinoma at an age between 1-32 years old. 97% of carcinomas are detected on the head or neck. Skin melanomas are seldom and complicate the freckles.
Very bad prognosis of xeroderma pigmentosum requests the execution of preventive measures and as much as possible the decrease of birth of children who shall appear with this syndrome. This is managed with provision of genetic nature advice and with prenatal diagnosis. To improve the prognosis we try to protect these people from the environmental factors which may spark the developing procedure and the appearance of carcinomas.